
Don't be embarrassed to talk about a bladder problem.
It can be embarrassing to talk to a doctor about Urinary Incontinence (UI) or Fecal Incontinence (FI) as there's a stigma around these hidden conditions which forces many to become prisoners in their own homes.
Don't be one of the millions of people who suffer in silence.
What is Urinary Incontinence? Simply put, it is the involuntary leakage of urine from the bladder. This could be just a few drops or a complete emptying of your bladder. The two most common types of urinary incontinence that affect women are Stress incontinence and Urge incontinence also called "Overactive bladder". If you have ever struggled to hold your urine during everyday life or physical activity you may suffer from UI.
Do You Know?

The two most common types of urinary incontinence are:
- Stress Incontinence: This is the most common type of incontinence. Stress incontinence happens when there is stress or pressure on the bladder due to weak pelvic floor muscles. Sudden actions such as Coughing, Sneezing, laughing, exercising and other physical activities can cause urine leakage. It is found to be more common in younger women.
- Urge Incontinence: With urge incontinence, urine leakage usually happens after a strong, sudden urge to urinate and before you can get to a bathroom. Urge incontinence is sometimes called “overactive bladder.” Urge incontinence is more common in older women and man.
Many women with urinary incontinence have both stress and urge incontinence. This is called “mixed” incontinence.
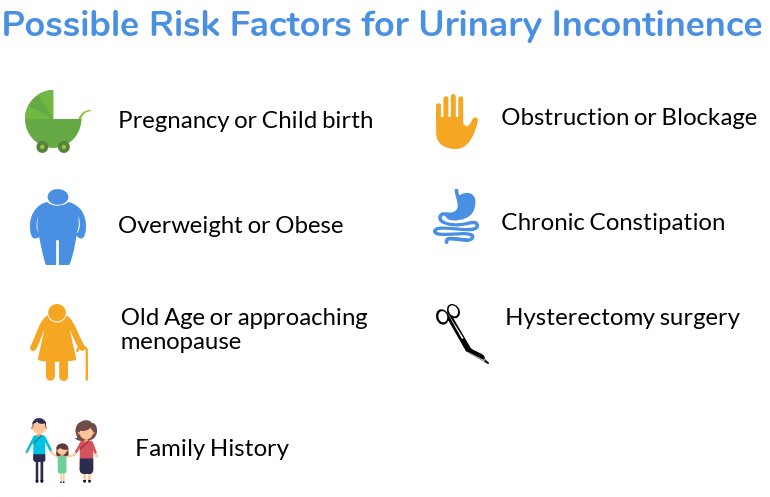
Living with Urinary Incontinence can affect your quality of life in multiple ways. Many people who experience suffer from lower self-esteem, discouraged physical activity and decreased independence.
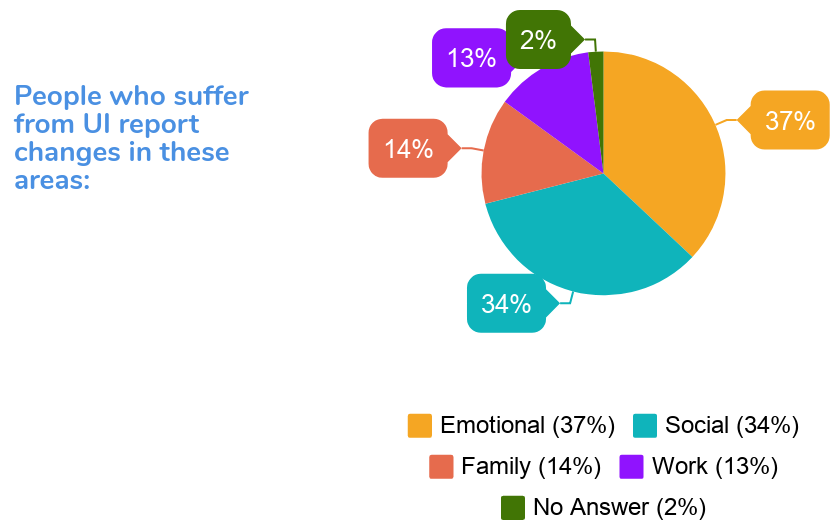
How is urinary incontinence treated?
Treatment for urinary incontinence depends on the type of incontinence, its severity, and the underlying cause. A combination of treatments may be needed.
A. Behavioral Techniques
- Bladder training — Bladder training can help you learn to go to the bathroom less frequently by "retraining" your bladder to hold more urine.
- Fluid and Diet Management - to regain control of your bladder. You may need to cut back on or avoid alcohol, caffeine or acidic foods.
B. Pelvic Floor Physiotherapy or Pelvic Floor Muscle Training- Follow the link for more details.
C. Lifestyle modification — Some changes in your lifestyle may help symptoms of urinary leakage.
- Weight loss – If you are overweight or obese, talk to your healthcare provider about strategies to lose weight. In people who are obese or overweight, losing weight often helps to reduce urine leakage in addition to improving other chronic medical conditions that are associated with incontinence (eg, diabetes and hypertension).
- Fluid management – If you drink large amounts of fluids, you may find that cutting back on fluids will reduce your leakage. A total of 64 ounces of all liquids (water, juice, milk, etc) per day is sufficient for most people; you may need more fluid when you are active and sweating or if it is hot. If you drink too little fluid, your urine may become very concentrated and darker than usual; this can irritate your bladder and increase the urgency to urinate.
- Avoiding constipation – Constipation can make urinary leakage worse. Increasing the amount of fiber in your diet to 30 grams per day may prevent constipation.
- Scheduled voiding – Emptying your bladder ("voiding") at regular intervals, rather than waiting until your bladder is very full, can decrease episodes of urgency incontinence and prevent stress leakage during physical activity with a full bladder. Try urinating every three to four hours regularly throughout the day.
D. Electrical Stimulation
E. Medications - Medications commonly prescribed to treat UI include Anticholinergics, Mirabegron (Myrbetriq), Alpha blockers, and Topical estrogen.
F. Medical Devices are also being used to treat UI such as Urethral insert-a small, tampon-like disposable device, and Pessary.
If other treatments prove unsuccessful, there are a variety of surgical procedures which can treat the problems that cause urinary incontinence. Most procedures help to keep the urethra or bladder neck closed, or provide support to the urethra and bladder neck in both Men and Women.
References:
- Seshan, V., & Muliira, J. K. (2013). Self-reported urinary incontinence and factors associated with symptom severity in community-dwelling adult women: implications for women’s health promotion. BMC Women’s Health, 13, 16. http://doi.org/10.1186/1472-6874-13-16.
- https://www.mayoclinic.org/diseases-conditions/urinary-incontinence/diagnosis-treatment/drc-20352814
