What You Should Know About Dry Needling
by Dr. Ankita Sharma, PT
What is Dry Needling?
It's a type of physical therapy developed by contemporary practitioners of Western medicine, where a thin filiform needle is inserted into a tight or painful area to create a micro-injury and trigger your body’s own healing response. Many injuries involve chronically tight, over-active muscles that just won’t let go, and/or nerve-related pain. In my experience, Dry Needling tends to be very effective in treating both of these types of issues.
This type of therapy may be particularly attractive for patients who are sensitive to pain medication or for those whose pain levels have not improved even after multiple session of other physical therapy, rest, exercise, or surgery. Dry needling increasingly has been finding usage among patients with chronic conditions that have resulted in long-lasting pain.
WHY IS IT CALLED DRY NEEDLING?
As opposed to a hypodermic needle used to give a flu shot or other type of injection, dry needles have no hollow tube in the center to inject liquid medication. Hence the name “Dry Needle”. This is because they’re used for a different purpose. As I mentioned above, the point of dry needling is to create a micro-injury to stimulate your own body’s healing response, rather than deliver a liquid medication.
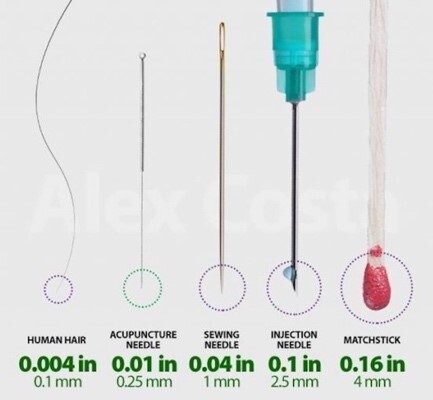
Because the dry needles are not hollow in the center, the diameter can be much smaller than a needle you would receive an injection with, as you can see in the picture below. If you’re a needle-phobe, this definitely makes a difference.
How is Dry Needling different from Acupuncture?
The most basic answer I give my patients is that “where you stick the needle and why” is the main difference between acupuncture and dry needling. There are certainly similarities, the biggest being that acupuncture and dry needles are one and the same.
However, there are also some major differences.
First, the philosophy is very different. Acupuncture originated in Asia thousands of years ago, and is based on restoring energy flow or “Chi” along specific pathways (meridians) in the body. A very wide range of conditions are treated by acupuncturists, ranging from allergies to depression to abdominal pain.
In contrast, Dry Needling is a much newer practice based on modern understanding of Human Anatomy and Physiology. With Dry Needling, the focus is on directly stimulating chronically sore or painful muscles or nerve pathways in the body to trigger the body’s own healing response. Treatments are focused on muscular and nerve-related issues, but not other body or mind issues (e.g. anxiety, depression, indigestion, allergies, etc.). Also unlike acupuncture, treatment is focused primarily on the area diagnosed as having dysfunction.
For example: If you have neck pain, Dry Needling treatment will usually consist of treatment entirely focusing around the neck region. Tight or over-active muscles and nerves will be diagnosed and targeted.
In contrast, with Acupuncture some needles may be placed at distant areas of the body as well, far away from the neck. Acupuncturists would likely also place needles in the neck in this case, but where they insert the needles will be based upon their understanding of restoring “Chi” and energy flow. That means different locations will likely be targeted, even within the neck, as compared to a practitioner performing Dry Needling.
Becoming a licensed acupuncturist requires specific training, typically over a period of around 3 years.
Training to practice Dry Needling can be incorporated into or after the formal education for a few different types of healthcare professionals including Physical Therapists, Physicians, and Chiropractors. Training for these professions is typically much shorter than for acupuncture, because all of these professions have already had extensive anatomy and physiology education as part of their schooling.
Does it hurt?
It varies. Some people don’t feel dry needling much at all and others have quite a bit of temporary discomfort.
For most people, the discomfort is temporarily moderate, but typically fades quickly over the course of a couple of minutes. The pain is typically less than getting something like a flu shot for most people as the needle is much smaller.
As far as what to expect after Dry Needling: most people experience some local muscle soreness, similar to that which you would have after working out, for up to 24 hours after the treatment. As you get up and get moving around the day after Dry Needling, most people begin to notice decreasing pain and improving function that surpasses the level they were at before the treatment.
What conditions can be treated with Dry Needling?
Dry needling therapy has been used throughout the world for years. It is an accepted treatment use by physiotherapists for the treatment of the following conditions and more:
- Acute and chronic injuries
- Headaches
- Neck and back pain
- Tendinitis
- Muscle spasms
- Sciatica
- Hip, knee and calf pain
- Muscle strains
- Fibromyalgia
- Elbow pain
- Knee Pain
- Overuse injuries
Is there any scientific evidence to support Dry Needling?
Absolutely. High quality evidence is already beginning to emerge for the use of Dry Needling in treating many different types of issues.
Shoulder pain (1), Neck Pain (2), Elbow Pain (3), Knee Pain (4), Low Back Pain (5), and Heel Pain/Plantar Fasciitis (6) are just a few of the body areas that have been studied and have shown Dry Needling to be of benefit in improving recovery when added to a physical therapy regimen.
Dry Needling has also been shown to be beneficial for reducing symptoms in many with neurological conditions, although its not used that widely.
Dry needling has also been shown to be beneficial in treating neck-related headaches (7).
I’ve only seen one study so far comparing acupuncture to dry needling. In this study, dry needling was more effective than acupuncture for low back pain in the immediate term, and equally effective as acupuncture after few weeks (5).
Overall, Dry Needling has been shown to be effective IF DONE ONLY BY TRAINED PROFESSIONAL in and of its own right in treating a variety of painful conditions across the body. However, its effects are almost always amplified when combined with exercise, stretching, education, and other hands-on treatments.
If you’re interested in Dry Needling treatment or would like to find out more, feel free to text or call us today at (+91) 8800639543. We’d love to help you get out of pain and back to doing the things you enjoy!




